Teresa's Story

Teresa, age 2, is a bubbly child who eagerly gives hugs and enjoys apple juice. The energetic toddler had a heart transplant on Christmas Day at Children’s National Hospital, and waited almost a year for a new heart.
She was diagnosed with dilated cardiomyopathy, which in Teresa's case, meant her enlarged heart lost its ability to pump blood effectively and is the leading cause for heart transplantation. She was treated a few times at the Emergency Department before doctors determined that her heart was beginning to fail. She was put on a Berlin Heart EXCOR® Pediatric Ventricular Assist Device (VAD) in March while she waited for almost a year for a heart.
“The Berlin Heart is great technology because it allows her to be up and out of bed and not on a ventilator. But, the longer a child is on the Berlin Heart, the greater the risk, like stroke or organ damage that would force us to take it out,” said Melissa Jones, CPNP-AC, Critical Care Nurse Practitioner, Cardiac Intensive Care Unit (Cardiac ICU) and VAD coordinator.
Waiting for a Heart
For almost nine months, the Berlin Heart worked as Teresa’s heart. Fortunately, she did not experience any complications such as pump failure or a stroke as the device pumped blood through her small body. Doctors say that about 30% of children using this device have a neurologic event, such as a stroke, during their time on support.
Jones helped to build the program devoted to managing patients on VAD such as Teresa, who was the longest patient at Children’s National on a VAD waiting for transplant.
“I was looking at pictures of her from several months ago and she has grown tremendously from when she got here,” Jones said. “When she first got here, we’d have to get her up out of bed and the occupational and physical therapy teams had to help her walk again, and now she’s dancing and jumping; we had to get her a helmet.”
Teresa was a delight to everyone she encountered in the Cardiac ICU.
“Everyone really loved her here; especially the other kids and parents,” Jones said. “She would walk down the unit and she was just such a joy and a ray of sunshine. She had a huge team that was really invested in her, really adored her, and put a lot of time and effort into making sure she didn’t any complications during her long stay.”
A Heart for Christmas
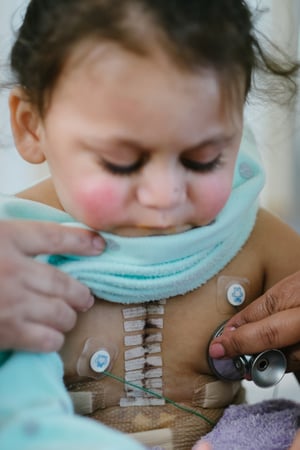 On Christmas Eve, a heart became available. A day before her nine-month anniversary on the mechanical heart, on Christmas Day, the Cardiac ICU team operated on Teresa to save her life.
On Christmas Eve, a heart became available. A day before her nine-month anniversary on the mechanical heart, on Christmas Day, the Cardiac ICU team operated on Teresa to save her life.
Janet Scheel, M.D., Director of the Advanced Cardiac Therapies and Heart Transplant Program explains that it took a long time to find Teresa a heart that matched.
“We hadn’t gotten many calls, so it was pretty exciting because it was Christmas Eve, it was such an amazingly good match – in terms of everything we knew about the donor, it’s the kind of match you don’t often get,” Dr. Scheel said. “It was like a Christmas present.”
On Christmas morning, multiple teams throughout the Washington, D.C., metropolitan area and within Children’s National, rallied to help Teresa, making arrangements to accept the heart offer. Many left their own families on Christmas Eve and Christmas Day to rush to the hospital.
Jones, who was the procurement nurse the day of the transplant, went to the airport to receive the heart.
“The feeling was overwhelming. I felt like that day, everybody was so excited in the unit, and the energy was incredible,” Jones said. “Everyone was so excited she was getting her heart because we’d been waiting so long. I got to work with such a big, dedicated team, and everyone really stepped up. You wouldn’t have known that people were away from their families at Christmas, everybody was just so happy to be a part of it.”
Jones opened Christmas presents with her sons, ages 3 and 5, before she left to pick up the heart Christmas morning.
“My husband had the idea to wake them at 4:30 in the morning and the boys didn’t care, they were so happy that Santa came. So, I was ready to go by 6 a.m. and the boys went back to bed with their Transformers in hand,” Jones said. “It was a rollercoaster of a day, but it was a privilege.”
Teresa’s surgery went well; she did not experience any complications. She was discharged in less than two weeks after her surgery. And although the transplant procedure went well, it will be a long journey for the spunky little girl.
“She will be followed very closely for the rest of her life. What we’ll be looking for are any signs that she has decreased heart function or coronary artery disease and it will be those things that tell us when she will need a new heart,” Dr. Scheel said. “But the quality of life we give these kids is great. I have a transplant patient who is high school quarterback, another who went to college and is on the swim team, and that’s what we do give them. We give them a quality of life and that’s worth it.”





